what color are tendons
Hi,welcome to solsarin site,today we want to talk about“what color are tendons”,
thank you for choosing us.
what color are tendons
Tendons are white. The white color is because they have little blood supply. Tendons don’t require a lot of blood because they’re not very active-they just connect your muscles to your bones. That’s why they’re classified as connective tissue. (In case you’re wondering, the average tendon uses 0.1 microliter of oxygen per milligram of dry tendon mass per hour. Now, aren’t you glad you know?)
Muscles are red. The red color is from their vast network of blood vessels. Muscles are very busy fellows, what with all of their contractions, so they need lots of blood to support their active lifestyle. The blood brings oxygen and nutrients and removes waste products from the muscles.

What’s this got to do with tendon repair?
The blood supply is the limiting factor in the repair of any injured tissue. Given their good supply of blood, injured muscles usually heal quickly. On the other hand, tendons are limited by their sparse blood supply. Consequently, they heal at a rather pokey pace.
Tendons are amazingly strong. Their tensile strength is greater than that of bone. In fact, fully contracted muscles have been known to break bones. (This is very unusual and is not caused by normal work motions.)
The force on a tendon increases as its muscle contracts. The highest level of tensile stress occurs when the muscle is fully contracted. The bigger the muscle, the greater the stress it can exert on its tendon.
If a tendon is stressed repeatedly and cannot recover quickly enough, the damage starts to accumulate. At first, the damage is microscopic. The collagen fibers of the tendon become damaged, the tendon starts to swell and thicken, which makes the situation worse. A vicious cycle begins. Damage causes swelling, which causes more damage.
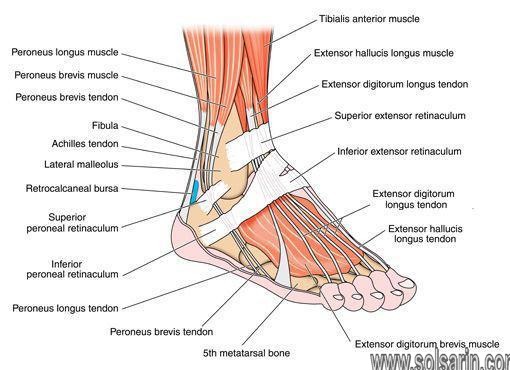
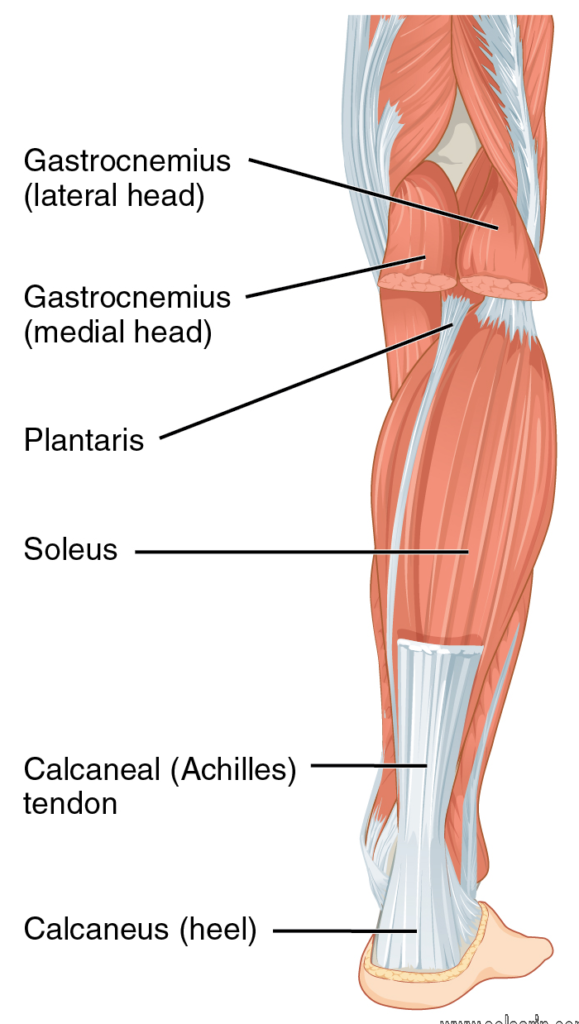
Overexertion injuries in tendons occur most often in the extremities. In the upper body, forceful or repetitive arm motions can lead to tennis elbow and golfer’s elbow. Rotator cuff tendinitis is another common injury and can develop if you work at shoulder level (or higher). In the legs, the most common type of tendinitis affects the Achilles tendon which attaches your calf muscles to your heel bone.
What is a tendon?
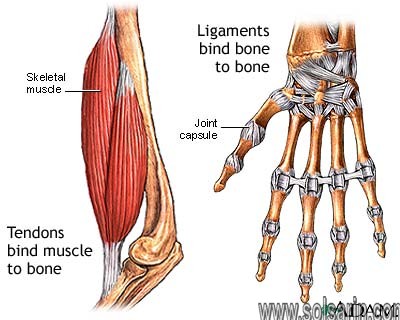
A tendon is a cord of strong, flexible tissue, similar to a rope. Tendons connect your muscles to your bones. Tendons let us move our limbs. They also help prevent muscle injury by absorbing some of the impact your muscles take when you run, jump or do other movements.
Your body contains thousands of tendons. You can find tendons from your head all the way down to your toes. The Achilles tendon, which connects your calf muscle to your heel bone, is the largest tendon in your body.
Tendons are highly resistant to tearing but aren’t stretchy. This means they can be easily injured when strained (stretched to point partial tearing of rope fibers) and may take a long time to heal.

Definition of Tendons
Tendon refers to a connective tissue that connects muscle to bone. Consequently, the tendon’s function is to make movement possible. Moreover, they are extremely resistant to tearing but are not extremely stretchy.
What are the parts of a tendon?
A tendon consists of:
- Endotenon: Connective tissue that surrounds the primary, secondary and tertiary fiber bundles. Helps the bundles glide against each other inside the tendon.
- Epitenon: Thin layer of connective tissue that surrounds the entire tendon.
- Paratenon: Loose layer of connective tissue that lets the tendon move against the epitenon and other tissues that the tendon touches. Located outside the epitenon.
- Sharpey fibers: Collagen fibers that attach the tendon to the bone.
- Sheath (synovium): Some tendons in the hand and foot have a sheath (synovium). This is the protective outer covering of the tendon. Produces a lubricating fluid called synovial fluid, which helps the tendon slide smoothly where it meets muscle and bone.
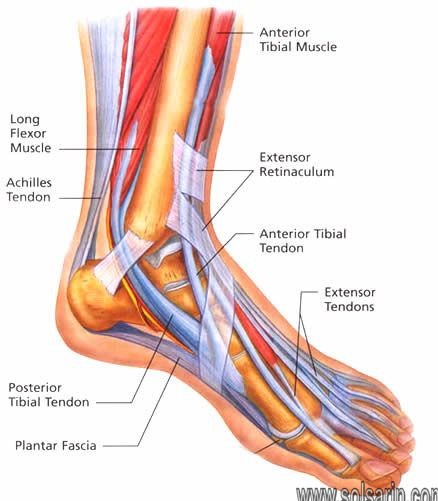
Anatomy
In addition to comprising the peritenon, some Tendons are covered by a synovial sheath in areas of mechanical stress or in areas requiring tendon constraint. Those tendons not covered by a synovival sheath are surrounded by a paratenon, consisting of loose connective tissue. Blood supply to tendons is scant, as opposed to that of muscle or bone, and it comes from the myotendinous junction, the tendon sheath or paratenon, and the enthesis. Peritendinous bursae occur at sites of potential tendon friction or compression (eg, where a tendon changes course, where a tendon may be compressed against a bone or another tendon)

Cellular Component of a Tendon
The tendon cells are known as tenoblasts and tenocytes. They make up approximately 90-95% of the cells within the tendon. The other 5-10% include the chondrocyctes, synovial cells and the vascular cells.
Tenoblasts are immature tendon cells. Initially they are different in size and shape but as they age they become elongated and spindle shaped and transform into tenocytes. The tenocyctes are responsible for the turnover of maintenance of the extracellular matrix (described below). The tenocyctes respond to mechanical load of the tendon and thus make adaptations. They are arranged in longitudinal rows and have extensive communication with adjacent cells usually through gap junctions.
Gap junctions are very complex and complicated structures. They have two hemi-channels. These are also called connexons (a collection of six connexin protein subunits). These have a central pore. The connexons in an open state allow metabolites and ions to pass freely between the gap junctions. moreover, the connexins are numbered, the ones which we are interested in for cell communication and tendon regeneration are connexins 26, 32 and 43.
Connexin 43 is situated in gap junctions between cells in rows along the collagen fibres. Connexins 26 and 32 have a more diffuse pattern. Connexin 43 is responsible for the inhibition of the collagen syntheses within the tenocyctes as a response to mechanical loading. Connexin 32 may have a stimulatory role, but all we need to know is that they aid communication between cells within the tendon to help with regeneration and adaptation.
Tendon Bursae
Tendon bursae help to minimize friction between the tendon and adjacent bone structures. These are small serous vesicles, located in the sites where a bony prominence can compress and then wear out the tendon; typical examples are subacromial, infrapatellar, and retrocalcaneal bursae.
Below the paratenon, the entire tendon is surrounded by a thin sheath of dense connective tissue called epitenonium. Together, these can be called peritenonium. Within the epitenonium the collagen fibrils are differently oriented, being disposed transversely as well as longitudinally and obliquely. Occasionally the epitenonium fibrils appear to be fused with the superficial tendon fibrils.
On its external surface the epitenonium is contiguous to the peritenonium, and on the inner surface, it is instead in continuity with the endotenonium, a thin membrane of loose connective tissue that covers the individual tendon fibers and groups them in larger units represented by bundles of fibers of various order. The function of endotenonium is to circumscribe, individualizing, the various orders of bundles and to allow the penetration and the capillary distribution of vasculonervous structures inside the tendon.
The point where the muscle pierces in the tendon is called muscle-tendon junction, while the point where the tendon inserts on the bone is called osteo-tendinous junction.

Acknowledgments
We sincerely thank Gerald Richardson (Dallas World Aquarium) for coordinating the research partnership with The Sloth Sanctuary of Costa Rica. Special thanks to Jesse Young (NEOMED) and Hazel Marie (YSU) for providing access to and assistance with use of the Instron machines.moreover, we thank Michael Granatosky (NYIT) for providing vervet monkey specimens. Thank you to two anonymous reviewers for very helpful comments. Thanks to Lydia Johnson, Abdel Yusuf, Branson Brownfield, Dakota Morgan, and Joshua Schlueter for assistance with data collection and analysis.
Portions of the work will be submitted as a Master Thesis by A.M.M. with a Cushwa/Commercial Shearing Fellowship providing support during AY 2019–2020. The YSU College of STEM, Office of Research, and Departments of Biological Sciences and Mechanical Engineering are acknowledged for their support of graduate student research. The Department of Neurobiology and Anatomy at NEOMED is also gratefully acknowledged.
More Details about Tendons
Tendons have fewer blood vessels in comparison to the muscles. Consequently, tendon injury can result when overstraining happens. Furthermore, tendons take a longer time to heal in comparison to the other types of tissues present in the body.
There is certainly a connection of bones to the muscles which is why the bones are able to move as the muscles tighten and relax. Moreover, in some parts of the body, there is a direct attachment of the muscle to the bone. However, this is not always the case because a suitable room may not be available on the bone, or the distance between bone and muscle may be too much.
Some tendons run through narrow tunnels whose formation takes place from ligaments and bones. Furthermore, there are some whose stretching takes place over the bumpy parts of bones like in the wrist and foot. Most noteworthy, the tendons in such places receive protection by tendon sheaths, which are layers of connective tissue.